Reading Time: 3 minutes

Median Arcuate Ligament Compression Syndrome (MALCS), a rare vascular disorder, affects a small percentage of the population. However, its impact on individuals can be significant, leading to chronic abdominal pain and other debilitating symptoms. This article aims to shed light on the incidence, symptoms, diagnosis, treatment options, post-surgical care, and preventive measures associated with MALCS.
Incidence: Although MALCS is considered uncommon, its true incidence remains uncertain due to its underdiagnosis. The condition primarily affects young to middle-aged individuals, with women being slightly more susceptible than men.
Symptoms: The hallmark symptom of MALCS is chronic, postprandial abdominal pain. Individuals often experience pain after meals, which may be severe and associated with weight loss, nausea, vomiting, and bloating. Other symptoms include fatigue, diarrhea, and a general decline in quality of life.
Diagnosis: Diagnosing MALCS can be challenging due to its non-specific symptoms. However, a combination of medical history, physical examination, and imaging studies can help in reaching a diagnosis.
Endoscopy: Endoscopy, such as an upper gastrointestinal (GI) endoscopy or colonoscopy, is often performed to rule out other possible causes of abdominal pain. These procedures allow direct visualization of the GI tract and can help identify any abnormalities.
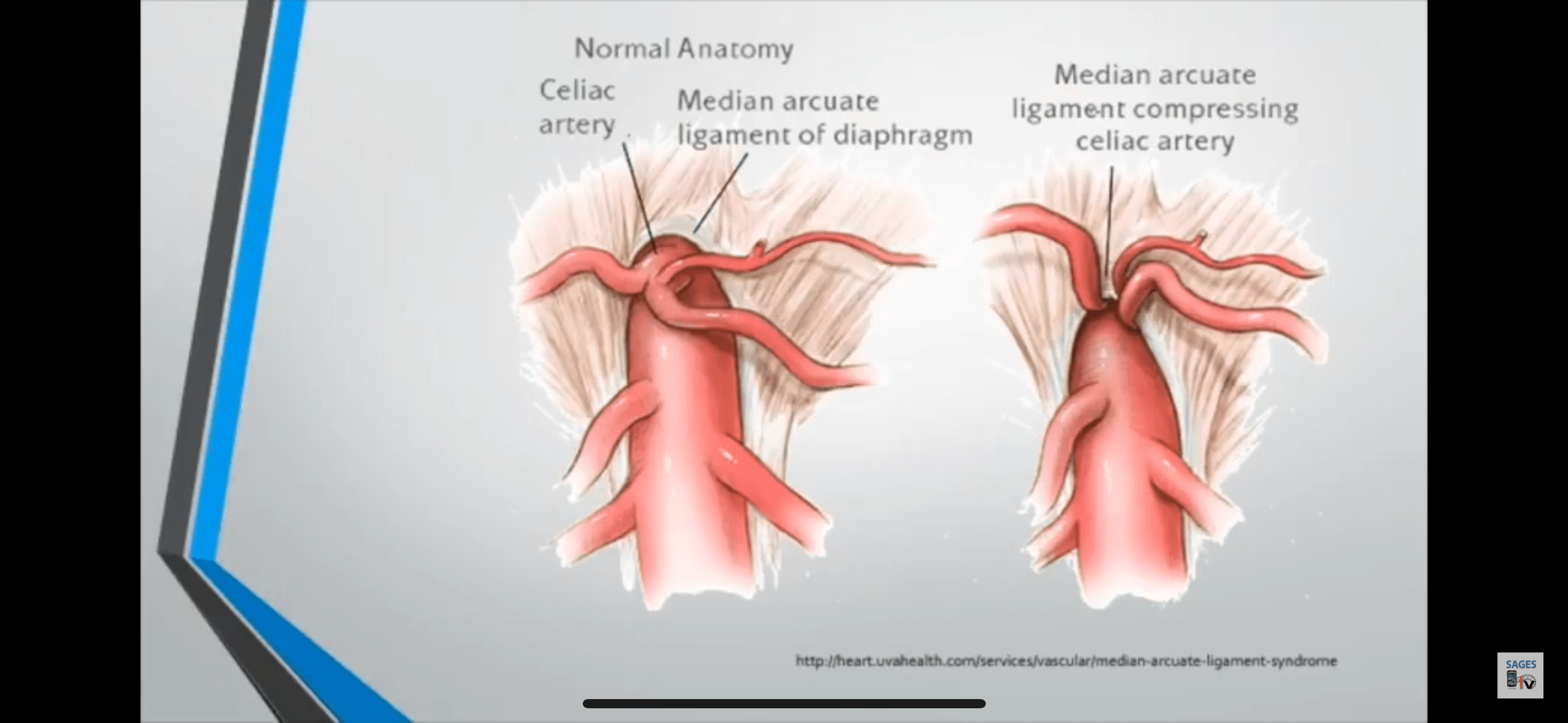
CT Scan: A computed tomography (CT) scan is commonly used to assess the anatomy of the abdominal region. It can reveal the compression of the coeliac artery by the median arcuate ligament, which is characteristic of MALCS. CT angiography may also be performed to evaluate blood flow to the affected area.
Doppler of Coeliac Artery: A Doppler ultrasound of the coeliac artery may be employed to assess blood flow through the narrowed vessel. This non-invasive imaging technique helps evaluate the severity of compression and aids in surgical planning.
Treatment: Conservative management, including dietary modifications and pain management, is typically the initial approach for MALCS. However, if symptoms persist or worsen, surgical intervention may be necessary to alleviate the compression and restore normal blood flow.
Surgery: The main surgical treatment for MALCS is called the median arcuate ligament release. This procedure involves dividing or removing the fibrous band that compresses the coeliac artery, relieving the constriction and improving blood flow. Laparoscopic approaches are preferred, as they are less invasive and have a shorter recovery time.
Results of Surgery: In most cases, surgical intervention for MALCS provides significant relief from symptoms. Patients often experience a reduction or complete resolution of abdominal pain and an improvement in their overall quality of life. However, individual outcomes may vary, and it is essential to discuss expectations and potential risks with the treating surgeon.
Care after Surgery: After undergoing a median arcuate ligament release, patients require careful postoperative care. This typically includes pain management, wound care, and gradually reintroducing a normal diet. Physical therapy may also be recommended to aid in recovery and restore strength and mobility.
Prevention: As the exact cause of MALCS remains unclear, there are no specific preventive measures known. However, maintaining a healthy lifestyle, including regular exercise, a balanced diet, and avoiding smoking, may contribute to overall vascular health and potentially reduce the risk of developing vascular disorders.
In conclusion, Median Arcuate Ligament Compression Syndrome is a rare vascular disorder that can significantly impact an individual’s quality of life. While diagnosis can be challenging, a combination of medical history, physical examination, and imaging studies can aid in identifying the condition. Surgical intervention often provides relief from symptoms, but postoperative care and follow-up are crucial for optimal recovery. Further research is needed to better understand the causes and potential preventive strategies for MALCS.
