Reading Time: 4 minutes
Gastroparesis
Summary: 30 Sec Read
- Introduction
- Brief overview of gastroparesis as a digestive disorder with delayed stomach emptying.
- Symptoms
- Nausea, vomiting, bloating, early satiety, heartburn, and reflux as common symptoms.
- Causes
- Neuromuscular disorders, vagus nerve damage, infections, and autoimmune conditions as primary causes.
- Complications if Untreated on Time
- Malnutrition, dehydration, blood sugar control issues, and reduced quality of life as potential complications.
- Diagnosis
- Diagnostic methods like medical history, physical examination, gastric emptying studies, and imaging tests.
- Treatment Options
- Dietary modifications, medications, enteral nutrition, and surgical intervention as treatment approaches.
- Home Remedies
- Practical tips for managing symptoms at home, including portion control and mindful eating.
- When to Consult a Doctor
- Indications for seeking medical advice, such as severe or persistent symptoms.
- When to Get Emergency Help
- Emergency situations, including severe dehydration and sudden abdominal pain, requiring immediate attention.
- Related Conditions
- Conditions with symptom overlap or links to gastroparesis, such as IBS, GERD, and diabetic gastroparesis.
- Prevention
- Strategies for minimizing risk, including diabetes management, dietary adherence, lifestyle choices, and early medical evaluation.
Introduction
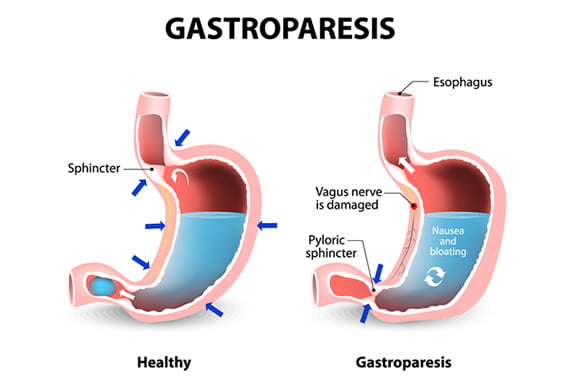
Gastroparesis, a relatively uncommon digestive disorder, can significantly impact an individual’s quality of life. Characterized by delayed stomach emptying, this condition often leads to uncomfortable and distressing symptoms. In this article, we will learn about gastroparesis, shedding light on its causes, potential complications, and the preventive measures individuals can take to manage and improve their condition.
Symptoms
Gastroparesis manifests through various distressing symptoms, including:
- Nausea and Vomiting: Frequent episodes of nausea and vomiting can disrupt daily life and lead to malnutrition and dehydration.
- Bloating and Abdominal Discomfort: Patients often experience bloating and discomfort after meals, even from small portions.
- Early Satiety and Reduced Appetite: Gastroparesis can cause individuals to feel full quickly, resulting in decreased food intake and potential weight loss.
- Heartburn and Reflux: Reflux symptoms, including heartburn and regurgitation, can be exacerbated by gastroperesis.
These symptoms can significantly impact one’s daily activities and overall well-being.
Causes
Understanding the underlying causes of gastroparesis is crucial for effective management. Some common causes include:
- Neuromuscular Disorders: Conditions that affect stomach muscles and nerves can disrupt the coordinated contractions required for proper digestion.
- Vagus Nerve Damage: Surgical procedures or long-term diabetes can damage the vagus nerve, which plays a vital role in digestive function.
- Infections and Autoimmune Conditions: Gastrointestinal infections or autoimmune diseases can harm the digestive system, leading to gastroparesis.
Complications if Untreated on Time
Neglecting gastroparesis can result in several complications:
- Severe Malnutrition: The inability to absorb nutrients due to delayed digestion can lead to malnutrition and weight loss.
- Dehydration and Electrolyte Imbalances: Persistent vomiting can cause dehydration and disrupt the body’s electrolyte balance.
- Aggravation of Underlying Conditions: For individuals with diabetes, poorly managed gastroparesis can complicate blood sugar control.
- Reduced Quality of Life: Chronic symptoms, including pain and discomfort, can diminish one’s quality of life.
Diagnosis
Diagnosing gastroparesis typically involves:
- Comprehensive Medical History: Healthcare professionals evaluate symptoms and medical history to identify potential risk factors.
- Physical Examination: A physical exam helps rule out other conditions and assess abdominal tenderness.
- Gastric Emptying Studies: Specialized tests, such as gastric emptying studies, confirm delayed stomach emptying.
- Imaging Tests: In some cases, CT scans or MRI may be necessary to detect structural issues within the digestive tract.
Treatment Options
Managing gastroparesis involves a multi-faceted approach, including:
- Dietary Modifications: Adopting a diet with smaller, more frequent meals and low-fiber foods can help ease symptoms.
- Medications: Physicians may prescribe medications to alleviate symptoms and improve stomach motility.
- Enteral Nutrition: Severe cases may require enteral nutrition through feeding tubes to ensure adequate nutrient intake.
- Surgical Intervention: For select patients, surgical procedures like gastric electrical stimulation (GES) may be considered.
Home Remedies
Individuals with gastroparesis can take proactive steps to manage their condition at home:
- Portion Control: Opt for smaller, balanced meals to minimize discomfort and promote digestion.
- Mindful Eating: Chew food thoroughly and eat slowly to aid digestion.
- Hydration: Maintain hydration with frequent sips of clear fluids throughout the day.
- Identify Trigger Foods: Recognize and avoid foods that exacerbate symptoms.
When to Consult a Doctor
If you have gastroparesis, seek medical advice in the following situations:
- Persistent and Severe Symptoms: Consult a healthcare professional if symptoms persist or worsen.
- Unintended Weight Loss: Rapid or unexplained weight loss should prompt a doctor’s visit.
- Signs of Dehydration: Dark urine, dry mouth, and extreme thirst indicate dehydration.
- Worsening Symptoms: If symptoms worsen despite home remedies, medical attention is crucial.
When to Get Emergency Help
Certain emergency situations require immediate medical assistance for gastroparesis patients:
- Severe Dehydration: Fainting, extreme weakness, or confusion can result from severe dehydration.
- Inability to Retain Fluids: If you can’t keep down fluids or medications, seek emergency care.
- Sudden and Severe Abdominal Pain: Intense abdominal pain or distension may indicate a serious issue.
- Overwhelming Weakness: If you experience overwhelming weakness or can’t stand, call for help immediately.
Related Conditions
Gastroparesis shares symptoms with or may be linked to other digestive conditions, including:
- Irritable Bowel Syndrome (IBS): Gastroparesis symptoms may overlap with IBS.
- Gastroesophageal Reflux Disease (GERD): Reflux symptoms can be aggravated by gastroparesis.
- Diabetic Gastroparesis: Individuals with diabetes are at increased risk of developing gastroparesis.
- Post-Viral Gastroparesis: Certain infections can trigger the development of gastroparesis.
Prevention
While not all cases of gastroparesis can be prevented, individuals can take steps to manage and potentially reduce their risk:
- Diabetes Management: For those with diabetes, strict blood sugar control can minimize the risk of gastroparesis.
- Dietary Adherence: Following dietary recommendations provided by healthcare professionals can help manage symptoms.
- Lifestyle Choices: Avoid excessive alcohol consumption and tobacco use, which can exacerbate gastroparesis.
- Early Medical Evaluation: Recognize potential risk factors and seek medical evaluation at the earliest signs of digestive issues.
Conclusion
Gastroparesis is a complex digestive disorder that can significantly impact one’s life. Understanding its causes, complications, and preventive strategies is essential for individuals affected by this condition. Early diagnosis, appropriate treatment, and lifestyle modifications can significantly improve their quality of life. For anyone experiencing gastroparesis symptoms, seeking medical advice promptly is the first step towards effective management and relief from discomfort.
